White House Unveils Anti-Fraud Crackdown Across Federal Programs
Vice President JD Vance launched the White House anti-fraud task force Friday, arguing the federal government has failed for decades to take fraud seriously.
THEN VS. NOW: He said the Trump administration will restore anti-fraud protections he claims were weakened under the Biden administration and implement a “whole-of-government approach” — requiring agencies to share data and coordinate efforts.
It comes as reporters and officials have found new cases of widespread fraud in multiple states, including Minnesota, California, New York, and Arizona, to name a few.
WHITE HOUSE’S AIM
The Trump administration says the goal of establishing an anti-fraud task force is to create a coordinated federal effort to detect, prevent, and prosecute fraud in major benefits programs like Medicaid, SNAP, and housing assistance.
Vance said the tragedy of government fraud is that taxpayer money meant to help families is instead going to fraudsters, leaving those in need without critical services.
"You have families who need these services who are unable to get them because people are getting rich off of fraud schemes instead of making sure that autistic children and their families get access to these resources," Vance said Friday.
STATES AT PLAY
The task force follows the viral Nick Shirley investigation into daycare and medical fraud in Minnesota from late last year. A fact sheet on the task force said, "There is strong reason to believe similar vulnerabilities exist in California, Illinois, New York, Maine, and Colorado, where insufficient safeguards and weak oversight increase the risk of large-scale fraud." Notably, those are largely Democratic-led states, but fraud exists across party lines.
MINNESOTA: Federal prosecutors estimate fraud schemes in the state could exceed $9 billion. The allegations include daycare centers taking millions in taxpayer funds without providing care, roughly $250 million in fake meal claims, and inflated billing tied to housing programs for seniors and people with disabilities.
Rewind: In 2021, federal investigators began uncovering pandemic relief beings used for multimillion-dollar fraud schemes. So far, nearly 100 people have faced charges.
State officials have pushed back on some claims — particularly those in the Shirley video — saying many daycares were operating as expected.
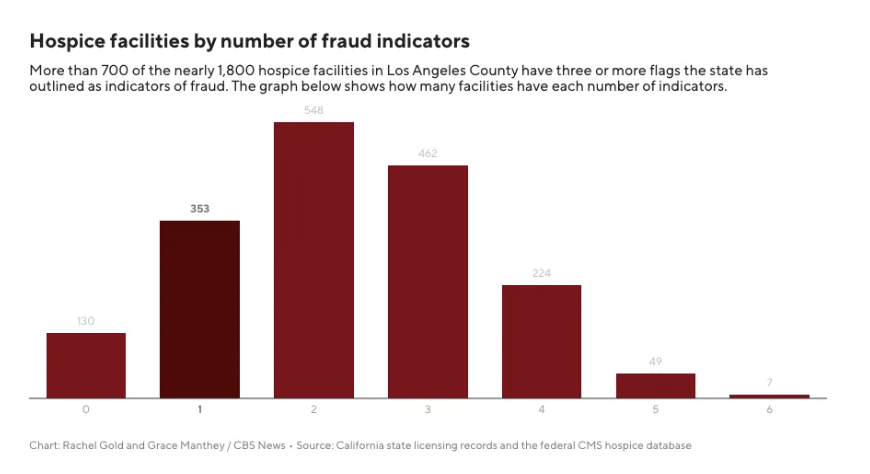
CALIFORNIA: CBS News investigations found that over 700 of the roughly 1,800 hospices in LA County triggered multiple red flags for fraud, including spotting that 89 ‘hospice' companies claim to operate out of one three-story building (see chart below). Recent reporting from Shirley on Medicare fraud tied to California’s hospice is also drawing congressional scrutiny. Rep. James Comer (R-KY) says as much as $3.5 billion may have been lost to fraud, with much of it tied to Los Angeles County.
California Governor Gavin Newsom’s office rejected claims the state is responsible for the fraud, noting that “Medicare is a FEDERALLY administered program” and that “California has been cracking down on fraud for YEARS — revoking 280+ hospice licenses and BANNED new ones beginning in 2022.”
FLORIDA: The federal government is also investigating Medicaid fraud in Florida, with the governor’s office vowing to cooperation in tackling the issue.
ALABAMA: Red states like Alabama are seeing some of the most widespread fraud. Alabama leads the nation with over 26,000 stolen SNAP claims, totaling about $10 million — more than California and New York.
The state moved late last year to roll out new cards that function like debit cards, aimed at making them harder to skim or clone.
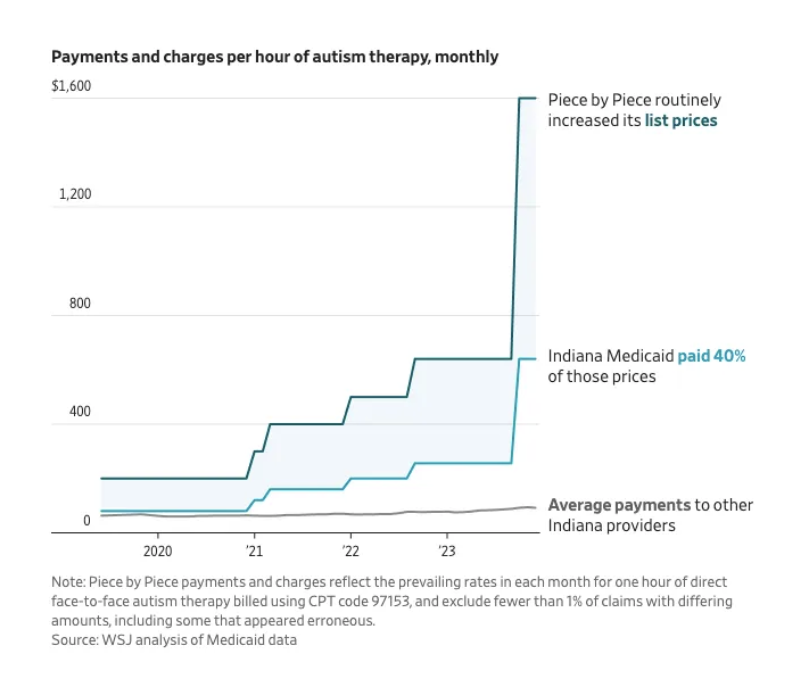
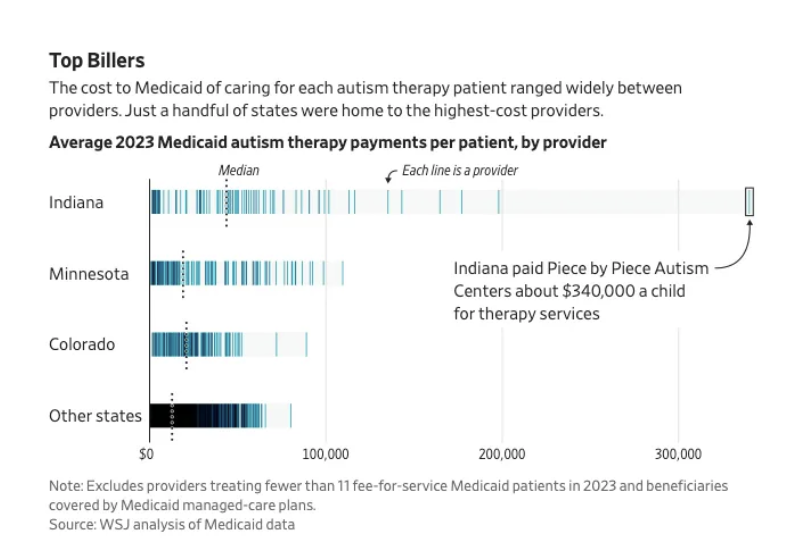
INDIANA: In Indiana, Piece by Piece Autism Centers is accused of exploiting Medicaid billing rules, receiving about $340,000 per patient at one point. From 2019 to 2023, Indiana directly paid the group roughly $58 million. The state has since barred the group’s providers from billing Medicaid.
BIGGER PICTURE: While recent reporting has highlighted some alarming cases, it remains unclear how widespread this is across the country.
Victor Hunt, CEO of home healthcare platform Zingage, told Stat News that 93% of Medicaid and Medicare providers show stable billing patterns, and even irregular cases don’t necessarily point to widespread fraud.